Groin hernia and you
- What is a groin hernia
- What causes groin hernia
- What are the symptoms
- How are groin hernias diagnosed
- Does my groin hernia need to be treated?
- What does surgery involve?
- Which operation should I have?
- When will I go home?
- What are the risks of surgery?
- How do I prepare for surgery?
- What happens when I go home?
- What should I watch out for in the first week following surgery?
What is a groin hernia?
A hernia is a defect (hole) in the abdominal muscles through which the abdominal contents (usually fat but sometimes intestines or other abdominal structures) can protrude. These occur at natural points of weakness in the muscles of the abdominal wall, usually in the inguinal (common), or femoral (less common) regions of the groin.
The term inguinal and femoral simply refer to the position in the groin where these hernias occur.
They can occur on one or both sides (bilateral) of the groin.
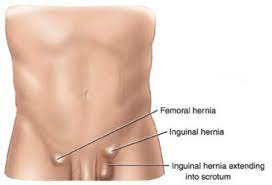
What causes a groin hernia?
Hernias may be present at birth, or develop in later life as a result of any factor that weakens the tissues of the abdominal wall (e.g. inherited genetics, increasing age, smoking, increased pressure within the abdomen – long term cough, §sustained heavy lifting).
Usually the development of a hernia is a combination of these factors. There is no good evidence that occasional heavy lifting is a risk factor for developing a hernia.
What are the symptoms of a groin hernia?
Remember a hernia is simply a hole in the abdominal wall – a hole through which something can protrude. The hole itself is not painful. There is sometimes, but not always, some discomfort– but it is not excruciating pain. So as a rule of thumb – if when you stand up or cough there is no swelling or a lump to see or feel – it is unlikely that you have a hernia – unlikely but not impossible.
When you lie down the protruding bit usually drops back through the hole and there is often nothing to see or feel – unless the hernia is stuck in the hole in the muscles. If the hernia doesn’t go back when you lie down this is called irreducible, (or sometimes incarcerated). That is why doctors examine you standing and coughing when checking for a hernia.
How are groin hernias diagnosed?
Most groin hernias are diagnosed by the clinical history and examination alone. Occasionally, if the diagnosis is unclear or if pain is the predominant symptom and there is no obvious swelling further investigations may be used. These include MRI scans, herniography and ultrasound scans. However, these scans have the problem that they may ‘over diagnose” hernias. In such cases they report a ‘possible’ or ‘small bulge’, which is really just a bit of normal tissue. So you can’t rely 100% on scans. Be guided by your surgeon.
Does my groin hernia need to be treated?
Although having a hernia is not usually a serious condition, hernias will not go away without surgical repair.
There is always the option to do nothing. This may be appropriate for longstanding hernias, which do not cause any symptoms and in patients with lots of other medical conditions. However, the majority of hernias will gradually become bigger and more uncomfortable with time, no matter how careful you are. Wearing a special device called a truss (support) to stop the lump coming out of the hole was used in the past, but is now thought to have no or limited benefit and are also fairly uncomfortable.